Chemotherapy is the use of medication (chemicals) to treat disease. More specifically, chemotherapy typically refers to the destruction of cancer cells. However, chemotherapy may also include the use of antibiotics or other medications to treat any illness or infection.

Factors that play a role in side effects include other ongoing treatments, previous health issues, age, and lifestyle. Some patients experience few side effects while others feel quite ill. Although most side effects clear up shortly after treatment ends, some may continue well after chemotherapy has ended, and some may never go away.
Chemotherapy drugs are most likely to affect cells in the digestive tract, hair follicles, bone marrow, mouth, and reproductive system. However, cells in any part of the body may be damaged.
Chemotherapy drugs work in various ways:
• Impairing mitosis (prevent cell division) – these are known as cytotoxic drugs.
• Targeting cancer cell’s food source,enzymes and hormones,require in order to grow
*Stopping the growth of new blood vessels that supply a tumor
Chemotherapy (chemo) drugs interfere with a cancer cell’s ability to divide and reproduce. Chemo drugs may be applied into the bloodstream to attack cancer cells throughout the body, or they can be delivered directly to specific cancer sites
.
When to get urgent medical advice
While the side effects of chemotherapy can be distressing, most do not pose a serious threat to your health.
However, occasionally some side effects can be very serious. For example, if you have a rapid fall in white blood cells, you may be vulnerable to a serious infection.
People having chemotherapy for cancer of their blood cells or bone marrow are most at risk of serious infections. This is because this type of cancer will already have caused a reduction in white blood cell numbers.
Symptoms of a serious problem include:
• a high temperature of 38°C (100.4°F) or above
• shivering
• breathing difficulties
• chest pain
• flu-like symptoms, such as muscle aches and pain
• bleeding gums or nose
• bleeding from other parts of the body that does not stop after applying pressure for 10 minutes
• mouth ulcers that stop you eating or drinking
*vomiting that continues despite taking anti-sickness medication
*four or more bowel movements a day, or diarrhoea
Circulatory and Immune Systems
Routine blood count monitoring is a crucial part of chemotherapy. That’s because the drugs can harm cells in the bone marrow, where blood is produced. This can result in several problems. Red blood cells carry oxygen to tissues. Anemia occurs when your body doesn’t produce enough red blood cells, making you feel extremely fatigued. Other symptoms of anemia include:
• lightheadedness
• pale skin
• difficulty thinking
• feeling cold
• general weakness
Chemo can lower your white blood cell count, which results in neutropenia. White blood cells play an important role in the immune system: they help fight infection and ward off illness. Symptoms aren’t always obvious, but a low white blood cell count raises the risk of infection and illness. People with an immune system weakened by chemotherapy must take precautions to avoid exposure to viruses, bacteria, and other germs.
Cells called platelets help the blood clot. A low platelet count, called thrombocytopenia, means you’re likely to bruise and bleed easily. Symptoms include nosebleeds, blood in vomit or stools, and heavier-than-normal menstruation.
Some chemo drugs can weaken the heart muscle, resulting in cardiomyopathy, or disturb the heart rhythm, causing arrhythmia. This can affect the heart’s ability to pump blood effectively. Some chemo drugs can increase the risk of heart attack. These problems are less likely to occur if your heart is strong and healthy at the start of chemotherapy.
Nervous and Muscular Systems
The central nervous system controls emotions, thought patterns, and coordination. Chemotherapy drugs may cause problems with memory, or make it difficult to concentrate or think clearly. This symptom sometimes is called “chemo fog,” or “chemo brain.” This mild cognitive impairment may go away following treatment, or may linger for years. Severe cases can add to anxiety and stress.
Some chemo drugs can cause pain, weakness, numbness, or tingling in the hands and feet (peripheral neuropathy). Muscles may feel tired, achy, or shaky. Reflexes and small motor skills may be slowed. It’s not unusual to experience problems with balance and coordination.
Digestive System
Some of the most common side effects of chemotherapy involve the digestive tract. Mouth sores and dry mouth can make it difficult to chew and swallow. Sores also may form on the tongue, lips, gums, or in the throat. Mouth sores can make you more susceptible to bleeding and infection. Many patients complain of a metallic taste in the mouth, or a yellow or white coating on the tongue. Food may taste unusual or unpleasant.
These powerful drugs can harm cells along the gastrointestinal tract. Nausea is a common symptom, and may result in bouts of vomiting. However, anti-nausea medications given in conjunction with chemotherapy drugs can help alleviate this symptom.
Other digestive issues include loose stools or diarrhea. In some people, hard stools and constipation can be a problem. This may be accompanied by pressure, bloating, and gas. Take care to avoid dehydration by drinking plenty of water throughout the day.
Side effects involving the digestive system can contribute to loss of appetite and feeling full even though you haven’t eaten much. Weight loss and general weakness are common. Despite all this, it’s important to continue eating healthy foods.
Hair, Skin, and Nails (Integumentary System)
Many chemotherapy drugs affect the hair follicles and can cause hair loss (alopecia) within a few weeks of the first treatment. Hair loss can occur on the head, eyebrows, eyelashes, and body. As troubling as it can be, hair loss is temporary. New hair growth usually begins several weeks after the final treatment.
Some patients experience minor skin irritations like dryness, itchiness, and rash. You may develop sensitivity to the sun, making it easier to burn. Your doctor can recommend topical ointments to soothe irritated skin.
Fingernails and toenails may turn brown or yellow, and become ridged or brittle. Nail growth may slow down, and nails may crack or break easily. In severe cases, they can actually separate from the nail bed. It’s important to take good care of your nails to avoid infection.
Sexual and Reproductive System
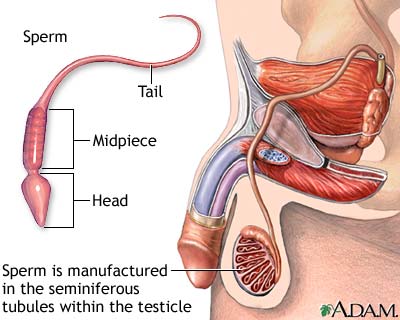
Chemotherapy drugs can have an effect on your hormones. In women, hormonal changes can bring on hot flashes, irregular periods, or sudden onset of menopause. They may become temporarily or permanently infertile. Women on chemotherapy may experience dryness of vaginal tissues that can make intercourse uncomfortable or painful. The chance of developing vaginal infections is increased. Chemotherapy drugs given during pregnancy can cause birth defects. In men, some chemo drugs can harm sperm or lower sperm count, and temporary or permanent infertility is possible.
Symptoms like fatigue, anxiety, and hormonal fluctuations may interfere with sex drive in both men and women. So can worrying about loss of hair and other changes in appearance. However, many people on chemotherapy continue to enjoy an intimate relationship and an active sex life.
Kidneys and Bladder (Excretory System)
The kidneys work to excrete the powerful chemotherapy drugs as they move through your body. In the process, some kidney and bladder cells can become irritated or damaged. Symptoms of kidney damage include decreased urination, swelling of the hands and feet (edema), and headache. Symptoms of bladder irritation include a feeling of burning when urinating and increased urinary frequency.
You’ll be advised to drink plenty of fluids to flush the medication from your system and to keep your system functioning properly. Note: Some medications cause urine to turn red or orange for a few days. This isn’t cause for concern.
Skeletal System
Most people—and especially women—lose some bone mass as they age. Some chemotherapy drugs can cause calcium levels to drop and contribute to bone loss. This can lead to cancer-related osteoporosis, especially in post-menopausal women and those whose menopause was brought on suddenly due to chemotherapy.
According to the National Institutes of Health (NIH), women who have been treated for breast cancer are at increased risk for osteoporosis and bone fracture. This is due to the combination of the drugs and the drop in estrogen levels. Osteoporosis increases the risk of bone fractures and breaks. The most common areas of the body to suffer breaks are the spine and pelvis, hips, and wrists.
Psychological and Emotional Toll
Living with cancer and dealing with chemotherapy can exact an emotional toll. You may feel fearful, stressed, or anxious about your appearance and your health. Some people may suffer from depression. Juggling work, financial, and family responsibilities while undergoing cancer treatment can become overwhelming.
Patients may receive monotherapy or combination therapy:
• Monotherapy – the patient is given just one drug.
• Combination therapy – the patient receives more than one drug.
Which type the patient receives will depend on the kind of cancer the patient has, as well as some other health considerations.
Chemotherapy may be given at different stages
• Neo-adjuvant therapy – if the tumor is large the surgeon may want to shrink it before surgery. This may involve some pre-operative chemotherapy and/or radiotherapy.
Chemoradiation therapy – the chemotherapy is given in combination with radiotherapy. Patients with localized Hodgkin’s lymphoma where the tumor is situated above the diaphragm should be given chemotherapy combined with radiotherapy,
How long is a course of chemotherapy?
In the majority of cases for best results the patient will need regular chemotherapy over a specific period. A protocol plan is drawn up which specifies when treatment sessions will occur and for how long.
A course of chemotherapy may be just a one-day treatment, or can last for a few weeks – it will depend on the type and stage of the cancer (how advanced it is). If the patient requires more than one course of treatment there will be a rest period for his/her body to recover. This could be a one-day treatment followed by a week’s rest period, followed by another one-day treatment followed by a three-week rest period, etc. This may be repeated many times.
Thanks to
http://www.medicalnewstoday.com/articles














![Studio_20150420_123131[1]](https://refomasisihat.files.wordpress.com/2015/04/studio_20150420_1231311.png?w=630&h=288)